Partnerships and Improved Strategic Information Scales Up Emergency Obstetric and Newborn Care in Kenya
- A mother and her child at a clinic in Kisumu County, Kenya. Photo by MEASURE Evaluation PIMA.
According to the World Health Organization, 800 women around the world die every day from pregnancy- or childbirth-related complications. Ninety-nine percent of those who die live in the developing world. While most complications develop during pregnancy, others can exist before pregnancy and be exacerbated by it. Major complications accounting for nearly 75 percent of all maternal deaths are:
Source: WHO
- Severe bleeding, mostly after childbirth;
- Infections, usually after childbirth; and
- High blood pressure during pregnancy (i.e. pre-eclampsia).
With a maternal mortality ratio (MMR) of 488 deaths per 100,000 live births,1 and as part of its efforts to achieve Millennium Development Goal 5, Kenya is committed to reducing its MMR to 147 deaths per 100,000 live births by 2015.2
The challenge is considerable. A 2009 survey on access to essential medicines in Kenya cited numerous barriers to the provision of emergency obstetric and newborn care (EmONC), including patient-related factors, as well as access, human resources, policy and infrastructure factors.3 Some patient-related barriers included low utilization of antenatal care and skilled deliveries, and poor knowledge, attitudes and practices. Additionally, even though the majority of Kenyans access care through public sector primary health facilities (e.g. dispensaries and health centers), which constitute 75 percent of the 4,433 public health facilities, almost a quarter of women (21 percent) felt it was not necessary to deliver in a hospital setting.
Moreover, only three percent of health facilities have the capacity to provide emergency obstetric care to address pregnancy-related complications, and access to essential services remains a serious challenge for most Kenyan women.4
In July 2013, USAID implementing partners (APHIAPLUS, AMPATHPLUS, MCHIP and MEASURE Evaluation PIMA [MEval-PIMA] and County Health Management Teams [CMHTs]) embarked on an initiative to scale up EmONC services to an initial 15 counties with high rates of maternal mortality, with varying results. Availability of quality data on EmONC is required to design interventions to address maternal and newborn complications at childbirth. EmONC is an integrated strategy aiming to equip health workers with skills, life-saving medicines, and equipment to manage the leading causes of maternal and newborn death.
A review of the first phase of the initiative was conducted in April 2014, with important lessons learnt that informed the technical and monitoring and evaluation (M&E) approaches adopted in the second phase. Overall, the key recommendations made for the success of the scale-up included a need for closer collaboration among partners, standardization of the support package offered to facilities, and standardization of the M&E tools, including the assessment and monitoring guidelines.
The revised approach led to a re-selection of target counties, a re-focus of the scope of support, and inclusion of the CHMTs in the decision-making processes. Implementing partners worked in consultation with USAID in providing guidelines and training on EmONC, as well as redistributing equipment. The M&E for the scale-up changed significantly, with MEval-PIMA taking the lead role in coordinating the review of assessment and monitoring tools and mechanisms to improve data quality, and training of partners and CHMT focal persons on assessment methods, tools, data analysis, interpretation of Excel-based dashboards, and data use for action planning.
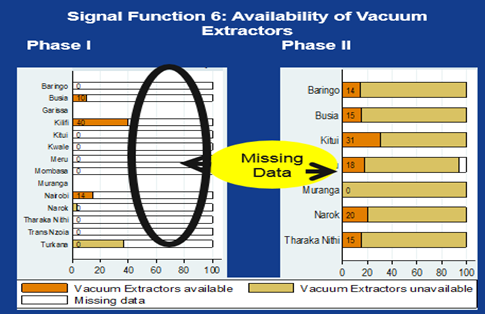
Unlike the first phase, in which data analysis was limited by significant levels of missing data (Figure 1), the second phase involved the design and standardization of data tools, and resolving the challenge of inadequate data capture, consolidation, and analysis – which made it possible to compare data across facilities and counties.
- Figure 1: Changes in data quality between phase 1 and phase 2, for which MEval-PIMA provided support
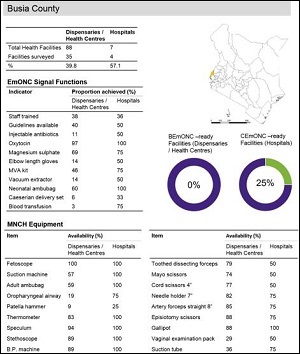
MEval-PIMA provides hands-on support for analysis and use of the dashboards, while facility-specific profiles provide evidence to focus activities from facility to county level (Figure 2).
- Figure 2: A sample county EmONC 2014 profile
Dr. Ruth Jahonga from USAID/ APHIAPLUS KAMILI, a USAID-funded project that supports scale-up in health facilities of the former Central and Eastern provinces of Kenya, explained the importance of EmONC.
“It is a strong advocacy package that can influence decision-making and resource mobilization. For example, using the package, we tracked some facilities that were supplied with vacuum-assisted delivery equipment that they weren’t using. We learnt that staff lacked confidence in using the equipment. To build that confidence, it was recommended to have staff visit and work alongside a mentor in a facility that was using the package. Without the tool we wouldn’t have identified this gap.”
The new tool has also led to increased county ownership of the findings, as demonstrated by CHMTs’ active involvement in data management and data use for action planning. This level of ownership has been realized by critically involving the CHMTs throughout the process in the spirit of true partnership.
References
- Kenya National Bureau of Statistics and ICF Macro. Kenya Demographic and Health Survey 2008-09. Calverton, Maryland: KNBS and ICF Macro, 2010.
- Ministry of Health. Health Sector Strategic Plan. Transforming Health: Accelerating attainment of Universal Health Coverage: The Kenya Health Sector Strategic Plan, July 2013 – June 2017. Nairobi: Ministry of Health, 2013.
- Ministry of Health. Access to Essential Medicines in Kenya: A Health Facility Survey. Nairobi: Ministry of Health, 2009.
- Ministry of Health. Kenya Service Availability and Readiness Assessment Mapping, 2013. Nairobi: Ministry of Health, 2014.
Useful resources
Ministry of Health. National Reproductive Health Strategy 2009 – 2015. Nairobi: Ministry of Health, 2009.
World Health Organization, UNFPA, UNICEF and Mailman School of Public Health. Averting Maternal Death and Disability: Monitoring emergency obstetric care; a Handbook. Geneva: World Health Organization, 2009.